It’s difficult to imagine that anyone is unaware of the coronavirus (SARS-CoV-2), which is causing a pandemic of COVID-19 disease. As uncertainty over this novel virus continues to build in the U.S. and globally, many Christians will turn to their churches for guidance on how to respond. The church needs to be prepared to respond with a calm, well-informed stance that quiets fearful hearts while invoking the most prudent courses of action.
It is important for church leadership to communicate calm based on the sovereignty of God. COVID-19 did not take God by surprise. God is accomplishing His plan specifically by using COVID-19 to upset the routines of people saved and unsaved. The unsaved may be unusually open to considering that their very breath is a gift from the God Who sent His Son to redeem them. God never wills that His people operate with a spirit of fear. We are to humble ourselves by rolling our anxiety on Him. Humble confidence in God does not mean that we are fatalists. “A prudent man foreseeth the evil, and hideth himself: but the simple pass on, and are punished” (Prov. 22:3). We take reasonable precautions to avoid the consequences of failing to act.
The practical issues at hand for churches revolve around the need to help stem the spread of SARS-CoV-2. The virus is spread through close contact with infected individuals, whether they display symptoms or not. Symptoms of infection include a fever, cough and shortness of breath. It is important not to see cases of the common cold as COVID-19, but to err on the side of caution where there is ambiguity. Large gatherings of people in close contact with one another greatly increase the opportunity for SARS-CoV-2 to spread through respiratory droplets produced when an infected person coughs or sneezes. Such droplets settle out of calm air fairly quickly. Someone may also become infected by touching a surface or object that has the virus on it (doorknobs, faucets, etc.) and then touching his mouth, nose or eyes.
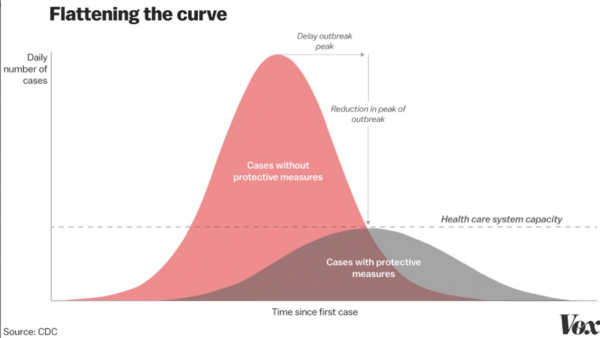
Epidemiologic studies are uncovering how COVID-19 is being spread over time. Anytime a population is exposed to a new virus, there is an initial period when nothing seems to be happening. With SARS-CoV-2, there is an average of five days between exposure and the start of symptoms. At five days following exposure, only half of those who will develop the illness will be showing symptoms. Those who have symptoms are most infectious during the first four days (before most show symptoms) but remain infectious for at least 10 days. The surge in infection in the days and weeks following the first case in an area has the potential to overwhelm the health care system as the graph below from the Centers for Disease Control makes clear. Protective measures are required to avoid overwhelming the health care system. Currently, the World Health Organization, CDC, and local public health departments are recommending that those who may have been exposed to the virus self-quarantine for 14 days.
Social Distancing
The CDC recommends “social distancing” or maintaining at least one meter of distance between people in a gathering. This certainly presents problems in a Sunday morning context. Sunday school classes in small classrooms might be temporarily replaced by combining classes and meeting in the auditorium. Certainly, you can encourage people to spread out in the auditorium as space permits. Definitely you should forgo, for now, handshakes and hugs. Encourage extended fellowship outside of the auditorium in the open air if possible. Church suppers are another type of assembly that might need to be temporarily disbanded during the pandemic. If you feel you must continue such suppers, have healthy people serve the food so that serving utensils are not handled by multiple people.
Caring for the Vulnerable
Most of the younger, healthy members in the church are not at high risk for complications from this infection, but this is an excellent opportunity for them to show love to those who are. The beloved elderly members are at higher risk of severe pneumonia. Anyone in the church family with a weakened immune system, lung diseases, cancer and other health problems are also at high risk.
Pastors could consider encouraging those members to participate through social media and virtual avenues during local infections. Pastors can help the congregation realize their opportunity to show love by protecting those who are the most vulnerable. Pastors should clearly communicate with members the concrete steps that should be taken. These include not attending church when you have an illness that could easily spread to others. Certainly, this applies to anyone who is ill and has symptoms that might be COVID-19.
Utilizing Virtual Alternatives
Some reading this will find that a congregant or a visitor to your assembly has tested positive for COVID-19 or has been in contact with someone who tests positive. In that event, it will be necessary for you to temporarily disband meeting together while the infection runs its course. You should submit to your local health department in this. Some state and local governments are currently mandating that church services not be held until the pandemic subsides.
If that is your situation, your decision has been made for you. In either of these situations you will need to find alternative means to keep your church body functioning as a body. How do you intend to support the weak, encourage the fainthearted, support one another in prayer, preach the Word, continue making disciples, etc.?
Small groups already in existence might be able to continue to function. If these groups can’t meet face-to-face, they can meet via conferencing software. One of the authors of this article met a small group session this week using free conferencing software as a feasibility test. Sermons could be posted to Sermon Audio or YouTube. In the most restrictive environment, a pastor could still preach, record and post a sermon.
Many churches communicate via e-mail or a church website and those channels can be exploited to keep the membership informed. Texting and e-mails from members to other members can fill in where a face-to-face meeting would have been preferable.
Supporting the Infected
How can the church best support members who become infected? If members should self-quarantine for two weeks, they will require support from the body of believers. They will likely need meals and groceries, and without adequate support, sick Christians may break quarantine and spread infection in the community. They will also need to have spiritual support in an extended time of isolation.
Observing Communion
What does COVID-19 mean for how we deliver communion? This sacred practice is vital to the health of the body of believers but is ripe for the spread of infection. If your church practices communion monthly or quarterly, you might consider forgoing it until the pandemic dies out in your area. If your church is still functioning normally and COVID-19 has yet to alter anything, you could make a few strategic alterations. Have deacons who will pass the bread and cup to adopt a few precautions. Before communion, each healthy deacon with no symptoms or exposure to infection should wash his hands with soap and warm water for at least 20 seconds. He should put on gloves and place the bread or the cup into the hand of each congregant to avoid contamination.
Singing Considerations
One more suggestion might be considered over the top by some. Singing can produce droplets that can be inhaled by those within a meter or so. You might consider temporarily replacing congregational singing with a solo from the platform. Choirs are likewise problematic as each vocalist can broadcast droplets to those immediately around him or her.
Taking Action Steps
Here are some concrete action steps that should be implemented regardless of any other actions you may choose to take:
- Stay home for 14 days if you have a cough or fever
- Greet each other with great love and compassion—but not a handshake!
- Wash your hands frequently with soap and warm water for at least 20 seconds
- Avoid close contact with other people by maintaining a meter distance
- Cover coughs and sneezes with your elbow or a tissue
Find more prevention tips on the CDC website.
The latest information about what BJU is doing to protect students, faculty and staff can be found at bju.edu/coronavirus.
This article was written special for BJUtoday by BJU professors Michael Gray, PhD (microbiology) and Amy Hicks, PhD, MPH (public health)